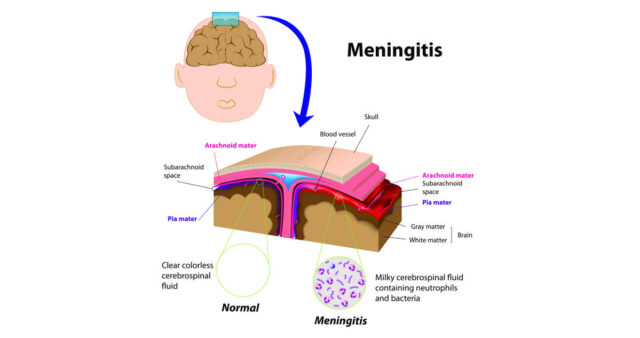
Meningitis is a serious and potentially life-threatening medical condition characterized by the inflammation of the protective membranes (meninges) surrounding the brain and spinal cord. It can be caused by bacterial, viral, fungal, or parasitic infections, but bacterial meningitis remains the most severe form due to its rapid progression and high mortality rate. Early diagnosis in meningitis cases is not just important it is often the difference between full recovery and severe complications or death. Among the cornerstone treatments, the ceftriaxone injection plays a vital role in managing bacterial meningitis effectively when administered promptly.
Understanding Meningitis and Its Severity
Meningitis symptoms can escalate quickly, often beginning with fever, headache, neck stiffness, nausea, vomiting, and sensitivity to light. In severe cases, patients may experience confusion, seizures, or loss of consciousness. Infants and young children may present differently, showing irritability, poor feeding, or a bulging fontanelle.
The rapid progression of bacterial meningitis makes it particularly dangerous. Pathogens such as Neisseria meningitidis, Streptococcus pneumoniae, and Haemophilus influenzae can invade the bloodstream and reach the meninges, causing inflammation that disrupts normal brain function. Without immediate medical intervention, this can lead to brain damage, hearing loss, or death within hours to days.
Why Early Diagnosis Matters
Early diagnosis is critical for several reasons:
- Prevention of Complications
Delayed diagnosis increases the risk of neurological complications such as cognitive impairment, motor deficits, and seizures. Early detection allows healthcare providers to initiate treatment before irreversible damage occurs. - Reduction in Mortality Rates
Bacterial meningitis has a high fatality rate if untreated. However, with early diagnosis and appropriate antibiotic therapy, survival rates improve significantly. - Timely Initiation of Targeted Therapy
Identifying the causative organism allows clinicians to tailor antibiotic therapy. While broad-spectrum antibiotics are started initially, laboratory confirmation ensures precise treatment. - Limiting Disease Transmission
Certain types of meningitis, especially meningococcal meningitis, are contagious. Early diagnosis enables public health interventions, including prophylactic treatment for close contacts.
Diagnostic Approaches
The diagnosis of meningitis involves a combination of clinical evaluation and laboratory tests:
- Lumbar Puncture (Spinal Tap): This is the gold standard for diagnosing meningitis. Cerebrospinal fluid (CSF) is analyzed for cell count, glucose, protein levels, and presence of pathogens.
- Blood Cultures: These help identify the causative organism in the bloodstream.
- Imaging Studies: CT scans or MRIs may be used to rule out other conditions or complications before performing a lumbar puncture.
- Polymerase Chain Reaction (PCR): This advanced test detects bacterial or viral DNA in CSF rapidly.
The key is not just accurate diagnosis but rapid diagnosis. Even a few hours’ delay can significantly worsen outcomes.
The Role of Ceftriaxone Injection in Treatment
Once meningitis is suspected, empirical antibiotic therapy must begin immediately often before laboratory confirmation. This is where the ceftriaxone injection becomes critically important.
Ceftriaxone is a third-generation cephalosporin antibiotic known for its broad-spectrum activity and excellent penetration into the cerebrospinal fluid. It is highly effective against many of the bacteria responsible for meningitis, including Neisseria meningitidis and Streptococcus pneumoniae.
Advantages of Ceftriaxone Injection:
- Broad-Spectrum Coverage: Effective against a wide range of gram-positive and gram-negative bacteria.
- Good CNS Penetration: Reaches therapeutic concentrations in the meninges, especially when they are inflamed.
- Convenient Dosing: Typically administered once or twice daily, improving compliance in hospital settings.
- Proven Efficacy: Widely recommended in clinical guidelines for the initial management of suspected bacterial meningitis.
In many treatment protocols, the ceftriaxone injection is combined with other antibiotics such as vancomycin to cover resistant strains until the exact pathogen is identified.
Impact of Delayed Treatment
Delays in administering antibiotics even by a few hours can have severe consequences. Studies have shown that each hour of delay in treatment increases mortality risk. Without early intervention using agents like ceftriaxone injection, the infection can rapidly worsen, leading to septic shock, brain swelling, and multi-organ failure.
Moreover, delayed treatment increases the likelihood of long-term complications such as:
- Hearing loss
- Memory problems
- Learning disabilities
- Epilepsy
These outcomes not only affect the patient’s quality of life but also place a significant burden on families and healthcare systems.
Special Considerations in High-Risk Groups
Certain populations are at higher risk of meningitis and require heightened vigilance:
- Infants and Young Children: Immature immune systems make them more susceptible.
- Elderly Individuals: Weakened immunity and comorbidities increase risk.
- Immunocompromised Patients: Conditions like HIV/AIDS or chemotherapy reduce the body’s ability to fight infections.
- People Living in Crowded Conditions: Such as dormitories or military barracks, where infections can spread easily.
In these groups, early diagnosis and immediate treatment with ceftriaxone injection can be life-saving.
Public Health and Awareness
Raising awareness about meningitis symptoms and the importance of early medical attention is crucial. Many cases are initially mistaken for less serious illnesses like the flu, leading to dangerous delays.
Vaccination also plays a key role in prevention. Vaccines against Haemophilus influenzae type b (Hib), Neisseria meningitidis, and Streptococcus pneumoniae have significantly reduced the incidence of meningitis worldwide. However, vaccination does not eliminate the need for early diagnosis and prompt treatment.
Conclusion
Meningitis remains a medical emergency that demands immediate attention. Early diagnosis is the cornerstone of effective management, enabling timely treatment that can prevent severe complications and save lives. The ceftriaxone injection stands out as a critical component in the initial treatment strategy, offering rapid and reliable antibacterial action against common meningitis pathogens.
Healthcare providers must maintain a high index of suspicion, especially in patients presenting with classic symptoms, and act swiftly. At the same time, public awareness and access to healthcare services must be improved to ensure that patients receive prompt diagnosis and treatment.
In the fight against meningitis, time is the most crucial factor and early diagnosis, supported by effective treatments like ceftriaxone injection, is the key to better outcomes.